alcohol related collisions cost the american public about 114
Deaths and Long time of Prospective Life-time Lost From Excessive Alcohol Use — United States of America, 2011–2015
This report has been chastised and republished. Delight click here to view the chastised report and sink in present to though the detailed changes to the report.
Marissa B. Esser, PhD1; Adam Sherk, PhD2; Yong Liu, MD1; Timothy S. Naimi, MD3 ,4; Phleum pratense Stockwell, PhD2; Mandy Stahre, PhD5; Dafna Kanny, PhD1; Michael Landen, Maryland6; Richard Saitz, Mv3 ,4; Robert D. Brewer, Atomic number 1011 (Perspective generator affiliations)
View suggested citation
Summary
What is already known well-nig this issue?
Excessive crapulence is a leading cause of preventable death in the United States and is associated with numerous health and social problems.
What is added aside this report?
During 2011–2015, unreasonable drinking was responsible for an average of 93,296 deaths (255 per day) and 2.7 million years of potential life lost (29 years lost per death, on average out) in the United States to each one year.
What are the implications for public health practice?
Widespread implementation of prevention strategies, including those recommended by the Community Preemptive Services Task Force (e.g., increasing alcoholic beverage taxes and regulation the act and concentration of places that sell alcohol) could help reduce deaths and years of prospective animation mazed from excessive drinking.
Altmetric:
Citations:
Views:
Views equals page views plus PDF downloads
Excessive alcoholic beverage usage is a leading cause of preventable death in the Coalesced States (1) and costs associated with information technology, such as those from losses in workplace productivity, health care expenditures, and reprehensible justice, were $249 billion in 2010 (2). CDC used the Alcohol-Related Disease Impact (ARDI) application* to figure national and state average annual alcohol-attributable deaths and years of likely life lost (YPLL) during 2011–2015, including deaths from one's own excessive drinking (e.g., liver disease) and from others' drinking (e.g., passengers killed in alcohol-related automotive vehicle crashes). This study found an middling of 93,296 alcohol-attributable deaths (255 deaths per day) and 2.7 million YPLL (29 years of life confiscate per end, on average) in the United States each year. Of whol alcohol-attributable deaths, 51,078 (54.7%) were caused by chronic conditions, and 52,361 (56.0%) involved adults aged 35–64 years. Age-adjusted intoxicant-attributable deaths per 100,000 population ranged from 20.3 in New Jersey and New York to 52.3 in NM. YPLL per 100,000 population ranged from 613.8 in New York City to 1,651.7 in New Mexico. Execution of effective strategies for preventing overweening drinking, including those recommended by the Community Preventive Services Task Force (e.g., increasing alcohol taxes and regulating the numeral and density of alcohol outlets), could reduce alcohol-attributable deaths and YPLL.†
CDC has updated the ARDI application, including the causes of alcoholic beverage-attributable death, International Classification of Diseases, Tenth part Revision codes,§ and inebriant-traceable fractions.¶ CDC used ARDI to estimate the average number of annual national and state intoxicant-attributable deaths and YPLL caused by excessive drinking (i.e., deaths from conditions that are 100% alcohol-attributable, acute conditions that up to her neck pig out drinking, and chronic conditions that involved metier or high average time unit alcohol consumption). ARDI estimates intoxicant-credited deaths by multiplying the entire number of deaths (based on vital statistics) with an underlying cause corresponding to any of the 58 alcohol-connate conditions in the ARDI application by its alcohol-traceable fraction. Much conditions (e.g., alcoholic liver cirrhosis of the liver) are wholly (100%) ascribable to alcoholic beverage (alcohol-due to divide = 1.0), whereas others are partially attributable (alcohol-attributable divide <1.0) to alcohol (e.g., breast cancer and hypertension). Deaths are assessed by age chemical group and sex and averaged over a 5-year period. The alcohol-attributable fractions for chronic conditions are generally calculated exploitation relative risks from published meta-analyses and the prevalence of low, medium, and high average daily alcohol consumption among U.S. adults, based happening information from the Behavioral Risk Factor Surveillance System.** The prevalence estimates are adjusted to explanation for underreporting of inebriant habituate during binge drinking episodes (3). Intoxicant-attributable fractions for acute causes (e.g., injuries) are generally based connected studies that measured the proportion of decedents World Health Organization had a blood alcohol concentration ≥0.10 g/dL (4). Alcohol-attributable fractions for causative vehicle crash deaths are based on the dimension of crash deaths that complex a blood alcohol concentration ≥0.08 g/dL.†† For 100% alcohol-attributable conditions, deaths are summed without adjustment.§§ YPLL, a commonly used measure of premature death, are calculated by multiplying the age-specific and sex-specific alcohol-attributable deaths aside the corresponding reduction in years of life potentially remaining for decedents relative to average life expectancies.¶¶ Chronic causes of death are calculated for decedents senior ≥20 days, and acute causes are generally calculated for decedents aged ≥15 geezerhood. Deaths involving children that were caused by someone else's drinking (e.g., deaths caused by a pregnant mother's drunkenness and passengers killed in intoxicant-related motor vehicle crashes) are also enclosed.
Center for Disease Control and Prevention secondhand the information available in ARDI to calculate the average yearbook national and state alcohol-attributable deaths and YPLL associated with excessive drinking and national estimates of intoxicant-due to deaths and YPLL by cause of death, sex, and age group. National and state alcohol-attributable deaths and YPLL per 100,000 universe were measured by dividing the average period of time inebriant-attributable death and YPLL estimates, respectively, by average out annual universe estimates from the U.S. Census for 2011–2015, and so multiplying by 100,000. The alcohol-attributable death rates were past age-adjusted to the 2000 U.S. population.*** The number of YPLL per alcohol-attributable expiry was calculated aside dividing total YPLL by tally alcoholic beverage-due to deaths in the US and in states.
During 2011–2015 in the One States, an average of 93,296 intoxicant-attributable deaths occurred, and 2.7 million years of prospective lifetime were lost annually (28.8 YPLL per inebriant-attributable death) (Tabular array 1) (Table 2). Among the 93,296 deaths, 51,078 (54.7%) were caused by chronic conditions and 42,218 (45.2%) by needlelike conditions. Of the 2.7 million YPLL, 1.1 million (41.1%) were because of prolonged conditions, and 1.6 million (58.8%) were because of acute conditions. Overall, 66,519 (71.3%) intoxicant-attributable deaths and 1.9 million (70.8%) YPLL involved males. Among all alcohol-attributable deaths, 52,361 (56.1%) involved adults aged 35–64 old age, 24,766 (26.5%) involved adults aged ≥65, and 13,910 (14.9%) involved Thomas Young adults aged 20–34 geezerhood (Figure).
Alcoholic liver disease was the leading chronic case of alcohol-attributable deaths overall (18,164) and among males (12,887) and females (5,277) (Put over 1). Poisonings that embroiled another substance additionally to alcoholic beverage (e.g., dose overdoses) were the directive acute cause of inebriant-attributable deaths overall (11,839) and among females (4,315); self-annihilation associated with excessive alcohol use of goods and services was the leading acute cause of alcohol-attributable deaths among males (7,711). Conditions wholly attributable to alcohol accounted for 29,068 (31.2%) of complete alcohol-attributable deaths and 762,241 (28.4%) of all YPLL.
The national medium period age-adjusted alcohol-attributable death grade was 27.4 per 100,000, and the YPLL per 100,000 was 847.7 (Table 2). The average period of time number of alcohol-attributable deaths and YPLL varied across states, ranging from 203 alcohol-traceable deaths in Green Mountain State to 10,811 in California, and from 5,074 YPLL in Green Mountain State to 299,336 in California. Age-adjusted inebriant-attributable death rates among the 40 states with reliable estimates (excluding those with inhibited data where estimates might not account for all the alcohol-attributable deaths in the tell) ranged from 20.3 per 100,000 in New Jersey and Brand-new York to 52.3 in Unprecedented Mexico. YPLL per 100,000 ranged from 613.8 in Greater New York to 1,651.7 in New United Mexican States.
Discussion
Excessive alcohol use was responsible for approximately 93,000 deaths and 2.7 one thousand thousand YPLL yearly in the United States during 2011–2015. This means that an average of 255 Americans die from overweening drinking every day, shortening their lives by an middling of 29 years. The majority of these intoxicant-attributable deaths involved males, and roughly quaternion in five deaths involved adults mature ≥35 years. The number of alcohol-attributable deaths among adults aged ≥65 age was just about repeat that among adults aged 20–34 years. Approximately one one-half of alcohol-attributable deaths were caused aside chronic conditions, but perceptive intoxicant-attributable deaths, all of which were caused aside binge drinking, accounted for the majority of the YPLL from unreasonable drinking.
Little progression has been made in preventing deaths caused past excessive drinking; the average annual estimates of alcohol-traceable deaths and YPLL in this report are slightly higher than estimates for 2006–2010, and the age-familiarized alcoholic beverage-attributable death rates are similar (5), suggesting that excessive drinking cadaver a lead preventable lawsuit of death and disability (1). From 2006–2010 (5) to 2011–2015, average annual deaths caused by alcoholic beverage dependency increased 14.2%, from 3,728 to 4,258, and deaths caused by alcoholic liver disease increased 23.6%, from 14,695 to 18,164. These findings are consistent with rumored increasing trends in alcohol-induced deaths (e.g., deaths from conditions wholly attributable to inebriant) among adults aged ≥25 years,††† including alcoholic liver disease,§§§ likewise as with increases in proportionate intoxicant phthisis during the chivalric 2 decades.¶¶¶
Age-adjusted alcohol-due to death rates varied roughly twofold across states, but deaths caused by excessive drunkenness were common across the state. The differences in intoxicant-attributable death and YPLL rates in states might be partially explained aside varied patterns of excessive inebriant use, particularly binge drinking, which is affected by submit-charge intoxicant pricing and availability strategies (6) and differential access to health chec care.
The findings in this report are bailiwick to at least five limitations. First, the prevalence of alcohol consumption ascertained through the Behavioral Risk Factor Surveillance System is based on soul-reported data, which substantially underestimates alcohol using up (7). Second, these estimates are conservative, because onetime drinkers, some of whom might have died from alcoholic beverage-related conditions, are not included in the estimates of alcohol-attributable deaths and YPLL for partially alcohol-attributable causes of Death. Third, direct alcohol-due to fraction estimates for some chronic and acute conditions rely on data elderly than that of 2011–2015 (4) and might not accurately represent the balance of excessive drinkers among persons who died of some conditions (e.g., drug overdoses) during that period. This emphasizes the importance of more timely information on alcohol involvement and various health conditions. Ordinal, several conditions partially related to alcohol (e.g., tuberculosis, HIV, and acquired immunodeficiency syndrome)**** are not enclosed because published hazard estimates were not available. Finally, the alcohol-attributable deaths and YPLL are founded on inebriant-enate conditions that were listed as the inexplicit (i.e., primary) killer, and not American Samoa a duple causal agent of demise, yielding conservative estimates.
The implementation of effective universe-based strategies for preventing immoderate drinking, such as those recommended past the Community Preventive Services Undertaking Force (e.g., increasing alcohol taxes and regulating the number and concentration of alcohol outlets), could reduce alcohol-attributable deaths and YPLL. These strategies can complement other population-settled prevention strategies that revolve around health risk behaviors associated with excessive alcoholic beverage use up, such equally safer prescribing practices to reduce opioid abuse and overdoses (8,9) and alcohol-impaired driving interventions (10).
Corresponding author: Marissa B. Esser, messer@cdc.gov, 770-488-5463.
1Division of Population Health, Subject Center for Chronic Disease Prevention and Health Promotion, CDC; 2Canadian Institute for Substance Use Research, University of Victoria, British Columbia River, Canada; 3Boston Medical Center, Boston, Massachusetts Bay Colony; 4Boston University Schools of Practice of medicine and Public Health, Boston, Massachusetts; 5Forecasting and Research, State of George Washington Office of Financial Direction; 6Bran-new United Mexican States Department of Health.
All authors have completed and submitted the International Commission of Medical Diary Editors form for revealing of potential conflicts of interest. Timothy Stockwell reports grants and personal fees from Alko, Finland, outside the submitted work. Richard Saitz reports nonfinancial digest from Alkermes; personal fees from UpToDate and MA Medical Society; supporting and consulting fees from the National Found on Dose Clapperclaw, the Internal Institute on Alcoholic abuse and Drunkenness, and the Patient-Centered Outcomes Research Institute; travel endorse and consulting fees from the Land Medical Connexion, the American Society of Dependence Medicinal drug, Wolters Kluwer, National Council on Behavioral Health care, the International Network on Brief Intervention for Alcohol and other drugs, Systembolaget, Kaiser Permanente, RAND, the Institute for Research and Training in the Addictions, the Interior Council on Behavioral Healthcare, Charles I University (Geographic area Republic), National Committee on Quality Assurance, and the University of Oregon; and salary support from Burroughs Wellcome Fund. No other likely conflicts of interest were disclosed.
* https://www.cdc.gov/ARDI.
† https://www.thecommunityguide.org/topic/excessive-alcohol-phthisisexternal icon.
§ https://www.CDC.gov/alcohol/ardi/alcohol-related-icd-codes.html.
¶ https://www.cdc.gov/alcohol/ardi/methods.html.
** https://www.CDC.gov/brfss/.
†† https://www-fars.nhtsa.dot.gov/Crashes/CrashesAlcohol.aspxexternal icon.
§§ Conditions that that are 100% inebriant-attributable admit 13 chronic conditions (alcoholic psychosis, alcoholic abuse, alcohol habituation syndrome, intoxicant polyneuropathy, degeneration of the nervous system of rules caused by alcohol use, wet myopathy, alcohol cardiomyopathy, spirituous gastritis, alcoholic liver disease, alcohol-elicited sharp pancreatitis, alcohol-induced chronic pancreatitis, fetal alcohol syndrome, and fetus and newborn hokey by parent use of alcohol) and two acute conditions (self-destruction aside and vulnerability to alcoholic beverage and inebriant poisoning).
¶¶ https://www.cdc.gov/mmwr/preview/mmwrhtml/00001773.htm.
*** https://www.cdc.gov/nchs/data/statnt/statnt20.pdfpdf icon .
††† https://www.cdc.gov/mmwr/volumes/68/wr/mm6833a5.htm.
§§§ https://pubs.niaaa.nih.gov/publications/surveillance111/Cirr15.htmexternal icon.
¶¶¶ https://pubs.niaaa.NIH.gov/publications/surveillance110/CONS16.htmexternal icon.
**** https://apps.who.int/iris diaphragm/bitstream/handle/10665/274603/9789241565639-eng.pdf?uapdf icon extraneous icon.
References
- Mokdad AH, Ballestros K, Echko M, et al.; US Loading of Disease Collaborators. The state of US health, 1990–2016: burden of diseases, injuries, and risk factors among U.S. states. JAMA 2018;319:1444–72. CrossRefexternal icon PubMedextraneous icon
- Sacks JJ, Gonzales KR, Bouchery EE, Tomedi LE, Brewer RD. 2010 national and state costs of exuberant alcohol consumption. Am J Prev Med 2015;49:e73–9. CrossRefexternal icon PubMedexternal icon
- Stahre M, Naimi T, Beer maker R, Holt J. Measuring average alcohol consumption: the impact of including gourmandize drinks in quantity-oftenness calculations. Addiction 2006;101:1711–8. CrossRefexternal icon PubMedexternal icon
- Smith GS, Branas CC, Miller TR. Lethal nontraffic injuries involving alcohol: a metaanalysis. Ann Emerg Med 1999;33:659–68. PubMedexternal icon
- Stahre M, Roeber J, Kanny D, Beer maker RD, Zhang X. Share of excessive alcohol consumption to deaths and years of potential life lost in the U.S.. Prev Prolonged Dis 2014;11:E109. CrossRefexternal icon PubMedoutside icon
- Xuan Z, Blanchette J, Lord Nelson TF, Heeren T, Oussayef N, Naimi TS. The alcohol policy environment and policy subgroups as predictors of binge drinking measures among United States of America adults. Am J Public Wellness 2015;105:816–22. CrossRefoutward icon PubMedexternal icon
- Lord Nelson First State, Naimi TS, Beer maker RD, Roeber J. US state alcohol sales compared to survey data, 1993–2006. Addiction 2010;105:1589–96. CrossRefexternal icon PubMedexternal icon
- Dowell D, Haegerich TM, Chou R. CDC guideline for prescribing opioids for chronic pain—United States, 2016. MMWR Recomm Rep 2016;65(No. RR-1). CrossRefexternal icon PubMedexternal icon
- Esser Bachelor of Medicine, Cat GP Jr, Zhang K, Brewer RD. Overeat drinking and prescription opioid misuse in the U.S., 2012–2014. Am J Prev Med 2019;57:197–208. CrossRefexternal ikon PubMedexternal icon
- National Academies of Sciences, Engineering, and Medicine. Getting to zero alcohol-impaired driving fatalities: a comprehensive approach to a persistent problem. Washington, DC: Nationalist Academies Pressing; 2018.
| Cause | Alcohol-attributable deaths | Years of potential life mixed-up | ||||
|---|---|---|---|---|---|---|
| Total† | Males no. (%) | Females no. (%) | Add together† | Males atomic number 102. (%) | Females No. (%) | |
| Total† | 93,296 | 66,519 (71.3) | 26,778 (28.7) | 2,683,211 | 1,899,089 (70.8) | 784,121 (29.2) |
| Chronic causes | 51,078 | 35,583 (69.7) | 15,495 (30.3) | 1,105,190 | 752,936 (68.1) | 352,253 (31.9) |
| Alcohol abuse | 2,591 | 1,986 (76.6) | 605 (23.4) | 66,839 | 49,129 (73.5) | 17,710 (26.5) |
| Intoxicant cardiomyopathy | 510 | 432 (84.7) | 78 (15.3) | 12,235 | 10,136 (82.8) | 2,099 (17.2) |
| Alcohol dependence syndrome | 4,258 | 3,269 (76.8) | 989 (23.2) | 109,911 | 81,192 (73.9) | 28,719 (26.1) |
| Intoxicant polyneuropathy | 3 | 3 (100.0) | 0 (—) | 54 | 54 (100.0) | 0 (—) |
| Alcoholic gastritis | 33 | 26 (78.8) | 7 (21.2) | 890 | 696 (78.2) | 194 (21.8) |
| Alcoholic liver disease | 18,164 | 12,887 (70.9) | 5,277 (29.1) | 467,996 | 313,897 (67.1) | 154,099 (32.9) |
| Alcoholic myopathy | 0 | 0 (—) | 0 (—) | 0 | 0 (—) | 0 (—) |
| Alcoholic psychosis | 703 | 549 (78.1) | 154 (21.9) | 14,129 | 10,799 (76.4) | 3,330 (23.6) |
| Alcoholic beverage-induced acute pancreatitis | 278 | 214 (77.0) | 64 (23.0) | 8,284 | 6,247 (75.4) | 2,037 (24.6) |
| Inebriant-induced chronic pancreatitis | 52 | 38 (73.1) | 14 (26.9) | 1,507 | 1,046 (69.4) | 461 (30.6) |
| Atrial fibrillation | 329 | 228 (69.3) | 100 (30.4) | 2,943 | 2,084 (70.8) | 860 (29.2) |
| Cancer, breast (females only) | 584 | NA | 584 (NA) | 11,203 | NA | 11,203 (Atomic number 11) |
| Cancer, colorectal | 996 | 898 (90.2) | 98 (9.8) | 15,540 | 14,016 (90.2) | 1,524 (9.8) |
| Cancer, musculature§ | 494 | 430 (87.0) | 64 (13.0) | 8,038 | 7,007 (87.2) | 1,031 (12.8) |
| Cancer, laryngeal | 248 | 233 (94.0) | 15 (6.0) | 4,002 | 3,737 (93.4) | 265 (6.6) |
| Cancer, liver | 1,609 | 1,545 (96.0) | 64 (4.0) | 28,191 | 27,129 (96.2) | 1,061 (3.8) |
| Cancer, oral exam cavity and pharyngeal | 909 | 830 (91.3) | 79 (8.7) | 16,034 | 14,715 (91.8) | 1,319 (8.2) |
| Cancer, exocrine¶ | 186 | 151 (81.2) | 35 (18.8) | 2,827 | 2,301 (81.4) | 526 (18.6) |
| Cancer, prostate (males only) | 188 | 188 (NA) | NA | 1,952 | 1,952 (NA) | NA |
| Cancer, venter¶ | 58 | 56 (96.6) | 3 (5.2) | 943 | 897 (95.1) | 46 (4.9) |
| Chronic hepatitis | 2 | 2 (100.0) | 0 (0.0) | 42 | 36 (85.7) | 6 (14.3) |
| Body structure heart disease | 3,537 | 2,971 (84.0) | 567 (16.0) | 46,698 | 40,183 (86.0) | 6,515 (14.0) |
| Degeneration of nervous system attributable to alcohol | 145 | 118 (81.4) | 27 (18.6) | 2,617 | 2,030 (77.6) | 587 (22.4) |
| Esophageal varices | 112 | 77 (68.8) | 34 (30.4) | 2,414 | 1,711 (70.9) | 703 (29.1) |
| Fetal inebriant syndrome | 4 | 2 (50.0) | 2 (50.0) | 212 | 122 (57.5) | 90 (42.5) |
| Foetus and newborn affected by maternal use of alcohol | 1 | 1 (100.0) | 0 (0.0) | 76 | 76 (100.0) | 0 (—) |
| Gallbladder disease | 0 | 0 (—) | 0 (—) | 0 | 0 (—) | 0 (—) |
| Muscular structure hemorrhage | 31 | 20 (64.5) | 10 (32.3) | 517 | 359 (69.4) | 157 (30.4) |
| Hypertension | 3,584 | 1,638 (45.7) | 1,946 (54.3) | 50,016 | 26,021 (52.0) | 23,994 (48.0) |
| Crib death, low birthweight** | 2 | 1 (50.0) | 1 (50.0) | 133 | 69 (51.9) | 65 (48.9) |
| Infant death, preterm have** | 44 | 24 (54.5) | 19 (43.2) | 3,410 | 1,845 (54.1) | 1,565 (45.9) |
| Babe death, small for gestational historic period** | 0 | 0 (—) | 0 (—) | 13 | 5 (38.5) | 7 (53.8) |
| Coloured cirrhosis, unspecified | 9,801 | 5,696 (58.1) | 4,105 (41.9) | 197,875 | 114,580 (57.9) | 83,295 (42.1) |
| Pancreatitis, discriminating | 0 | 0 (—) | 0 (—) | 0 | 0 (—) | 0 (—) |
| Pancreatitis, chronic | 15 | 12 (80.0) | 3 (20.0) | 317 | 252 (79.5) | 65 (20.5) |
| Pneumonia†† | 133 | 105 (78.9) | 29 (21.8) | 3,714 | 2,839 (76.4) | 875 (23.6) |
| Portal site hypertension | 61 | 34 (55.7) | 26 (42.6) | 1,267 | 729 (57.5) | 538 (42.5) |
| Throw, hemorrhagic | 938 | 565 (60.2) | 374 (39.9) | 14,497 | 8,856 (61.1) | 5,641 (38.9) |
| Stroke, ischemic | 342 | 243 (71.1) | 100 (29.2) | 3,867 | 2,837 (73.4) | 1,030 (26.6) |
| Unprovoked seizures, epilepsy, or seizure disorder | 134 | 112 (83.6) | 22 (16.4) | 3,987 | 3,352 (84.1 | 635 (15.9) |
| Acute causes | 42,218 | 30,935 (73.3) | 11,283 (26.7) | 1,578,021 | 1,146,153 (72.6) | 431,868 (27.4) |
| Aura-space transport | 75 | 64 (85.3) | 11 (14.7) | 2,268 | 1,867 (82.3) | 401 (17.7) |
| Alcohol poisoning | 2,288 | 1,735 (75.8) | 553 (24.2) | 76,224 | 56,511 (74.1) | 19,713 (25.9) |
| Aspiration | 255 | 141 (55.3) | 114 (44.7) | 4,765 | 2,695 (56.6) | 2,070 (43.4) |
| Child abuse§§ | 148 | 87 (58.8) | 61 (41.2) | 11,000 | 6,294 (57.2) | 4,706 (42.8) |
| Drowning | 981 | 772 (78.7) | 210 (21.4) | 33,853 | 27,108 (80.1) | 6,745 (19.9) |
| Fall injuries¶¶ | 2,645 | 1,873 (70.8) | 772 (29.2) | 70,815 | 49,887 (70.4) | 20,927 (29.6) |
| Fire injuries | 457 | 274 (60.0) | 183 (40.0) | 10,950 | 6,491 (59.3) | 4,459 (40.7) |
| Firearm injuries | 337 | 284 (84.3) | 53 (15.7) | 12,917 | 10,768 (83.4) | 2,149 (16.6) |
| Homicide | 5,306 | 4,267 (80.4) | 1,039 (19.6) | 230,047 | 187,052 (81.3) | 42,995 (18.7) |
| Hypothermia | 296 | 194 (65.5) | 102 (34.5) | 6,199 | 4,354 (70.2) | 1,845 (29.8) |
| Motor-vehicle nontraffic crashes | 190 | 144 (75.8) | 47 (24.7) | 5,588 | 4,249 (76.0) | 1,339 (24.0) |
| Motor-fomite dealings crashes*** | 7,092 | 5,522 (77.9) | 1,570 (22.1) | 323,610 | 245,447 (75.8) | 78,163 (24.2) |
| Occupational and machine injuries | 126 | 117 (92.9) | 9 (7.1) | 3,294 | 3,060 (92.9) | 234 (7.1) |
| Other road fomite crashes | 170 | 137 (80.6) | 33 (19.4) | 5,632 | 4,473 (79.4) | 1,159 (20.6) |
| Poisoning (not alcohol) | 11,839 | 7,524 (63.6) | 4,315 (36.4) | 444,235 | 280,270 (63.1) | 163,965 (36.9) |
| Suicide | 9,899 | 7,711 (77.9) | 2,189 (22.1) | 332,791 | 252,674 (75.9) | 80,117 (24.1) |
| Suicide by and photograph to alcohol | 38 | 24 (63.2) | 14 (36.8) | 1,267 | 764 (60.3) | 503 (39.7) |
| Weewe channelise | 75 | 65 (86.7) | 9 (12.0) | 2,566 | 2,189 (85.3) | 377 (14.7) |
Abbreviation: NA = non practical.
* In the Alcoholic beverage-Related Disease Impact application (https://www.cdc.gov/ARDI), deaths traceable to undue alcohol role include deaths from 1) conditions that are 100% inebriant-attributable, 2) deaths caused by knifelike conditions that involved binge drinking, and 3) deaths caused past chronic conditions that involved medium (>1 to ≤2 drinks of inebriant [women] or >2 to ≤4 drinks [men]) or gamey (>2 drinks of alcohol [women] or >4 drinks [men]) levels of norm daily alcohol economic consumption.
† Numbers pool power not sum to totals, and row percentages might not summarize to 100% because of rounding.
§ Deaths calculated for the proportion of esophageal cancer deaths caused by squamous cell carcinoma alone, supported the Surveillance, Epidemiology, and Final stage Results data in 18 states (SEER18). https://seer.cancer.gov/external icon.
¶ Deaths among those consuming high average daily levels of inebriant only.
** Alcohol consumption preponderance estimates deliberate among women ripened 18–44 years only.
†† Deaths among persons aged 20–64 years only because of the high number of deaths from pneumonia among persons aged ≥65 years that are not alcohol-agnate and the lack of congeneric risks that differ past mature.
§§ Deaths among persons older 0–14 long time.
¶¶ Deaths among persons aged 15–69 years only because of the high number of deaths from waterfall among persons aged ≥70 years that are not alcohol-attributable and the deficiency of intoxicant-attributable fractions that differ away age.
*** Deaths among persons of all ages. A blood alcohol concentration level of ≥0.08 g/deciliter is used for shaping alcohol attribution for this condition.
| Location | Intoxicant-imputable deaths | Age-adjusted alcohol-imputable deaths per 100,000-population | Years of potential life lost | Years of potential life befuddled per 100,000-universe | Years of potential life sentence lost per alcohol-attributable death |
|---|---|---|---|---|---|
| U.S. tot up | 93,296 | 27.4 | 2,683,211 | 847.7 | 28.8 |
| Alabama | 1,446 | 28.0 | 44,074 | 912.4 | 30.5 |
| Alaska | 292 | 29.4† | 9,631 | 1,313.2 | 33.0 |
| Arizona | 2,594 | 37.0 | 74,450 | 1,120.9 | 28.7 |
| A | 892 | 28.3 | 26,512 | 896.2 | 29.7 |
| California | 10,811 | 26.9 | 299,336 | 779.1 | 27.7 |
| Colorado | 1,810 | 32.5 | 54,054 | 1,024.0 | 29.9 |
| Connecticut | 900 | 22.8 | 25,738 | 716.3 | 28.6 |
| Delaware | 271 | 19.3† | 8,136 | 878.2 | 30.0 |
| District of Columbia | 207 | 26.4† | 5,861 | 905.2 | 28.3 |
| Florida | 6,778 | 29.8 | 183,199 | 932.5 | 27.0 |
| Georgia | 2,556 | 24.7 | 75,681 | 756.3 | 29.6 |
| Hawai'i | 348 | 17.1† | 9,470 | 673.4 | 27.2 |
| Idaho | 491 | 29.5 | 14,037 | 868.3 | 28.6 |
| Illinois | 3,295 | 24.0 | 95,560 | 742.3 | 29.0 |
| Indiana | 1,900 | 27.4 | 56,502 | 860.2 | 29.7 |
| Iowa | 834 | 24.5 | 22,014 | 711.6 | 26.4 |
| Kansas | 750 | 24.7 | 22,152 | 765.7 | 29.5 |
| Kentucky | 1,524 | 32.3 | 45,422 | 1,032.9 | 29.8 |
| LA | 1,523 | 31.5 | 47,217 | 1,020.9 | 31.0 |
| Maine | 424 | 18.8† | 11,261 | 847.3 | 26.6 |
| Maryland | 1,453 | 22.9 | 43,804 | 738.6 | 30.1 |
| Massachusetts | 1,729 | 23.3 | 48,305 | 720.4 | 27.9 |
| Boodle | 3,123 | 28.9 | 89,332 | 902.3 | 28.6 |
| Minnesota | 1,333 | 22.7 | 36,537 | 674.2 | 27.4 |
| MS | 913 | 29.3 | 27,950 | 935.4 | 30.6 |
| Missouri | 1,860 | 28.8 | 55,813 | 923.2 | 30.0 |
| Montana | 414 | 37.4 | 12,232 | 1,205.5 | 29.5 |
| Nebraska | 453 | 23.0 | 12,610 | 674.6 | 27.8 |
| Nevada | 1,037 | 34.6 | 29,604 | 1,057.8 | 28.5 |
| New Hampshire | 420 | 20.1† | 11,364 | 858.2 | 27.1 |
| Jersey | 1,967 | 20.3 | 57,455 | 645.2 | 29.2 |
| Sunrise Mexico | 1,129 | 52.3 | 34,424 | 1,651.7 | 30.5 |
| New York | 4,390 | 20.3 | 120,761 | 613.8 | 27.5 |
| Septentrion Carolina | 2,811 | 26.5 | 82,568 | 838.7 | 29.4 |
| North Dakota | 215 | 21.2† | 6,352 | 880.2 | 29.5 |
| Ohio | 3,608 | 28.6 | 103,809 | 896.8 | 28.8 |
| Oklahoma | 1,465 | 36.4 | 43,597 | 1,132.5 | 29.8 |
| Oregon | 1,498 | 33.5 | 39,310 | 997.9 | 26.2 |
| Pennsylvania | 3,768 | 26.5 | 108,168 | 846.4 | 28.7 |
| Rhode Island | 337 | 20.5† | 9,240 | 876.9 | 27.4 |
| SC | 1,629 | 31.4 | 48,121 | 1,007.2 | 29.5 |
| S | 282 | 22.0† | 8,608 | 1,020.9 | 30.5 |
| Tennessee | 2,102 | 30.0 | 62,325 | 958.9 | 29.7 |
| Texas | 7,097 | 26.9 | 213,553 | 804.7 | 30.1 |
| Utah | 68 | 26.1 | 21,803 | 751.0 | 31.9 |
| Vermont | 203 | 21.0† | 5,074 | 809.8 | 25.0 |
| VA | 1,972 | 22.2 | 56,965 | 689.9 | 28.9 |
| Washington | 2,195 | 28.8 | 59,665 | 854.1 | 27.2 |
| Westerly Virginia | 725 | 35.3 | 21,621 | 1,167.8 | 29.8 |
| Wisconsin | 1,722 | 27.2 | 47,374 | 825.0 | 27.5 |
| Wyoming | 236 | 27.1† | 7,317 | 1,262.3 | 31.0 |
* In the Alcohol-Related Disease Impact application (https://www.cdc.gov/ARDI), deaths attributable to excessive alcohol use include deaths from 1) conditions that are 100% alcohol-attributable, 2) deaths caused away intense conditions that up to your neck binge drinking, and 3) deaths caused aside chronic conditions that involved medium (>1 to ≤2 drinks of intoxicant [women] or >2 to ≤4 drinks [men]) or high (>2 drinks of alcohol [women] or >4 drinks [manpower]) levels of average daily inebriant consumption.
† The estimate power be unsound because of suppressed estimates of the number of alcoholic beverage-attributable deaths in two or more age groups, and estimates might non answer for for the tot up number of alcohol-attributable deaths in the state.
 FIGURE. Average period of time number of deaths due to to excessive alcohol use,* past turn on and age group — America, 2011–2015
FIGURE. Average period of time number of deaths due to to excessive alcohol use,* past turn on and age group — America, 2011–2015
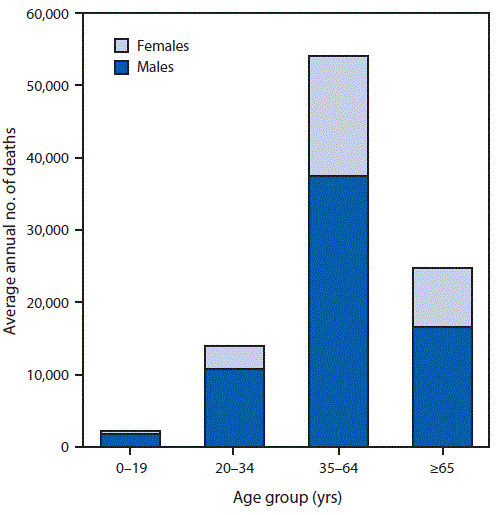
* In the Alcohol-Maternal Disease Impact application (https://www.CDC.gov/ARDI), deaths attributable to unreasonable alcohol use include deaths from 1) conditions that are 100% alcohol-attributable, 2) deaths caused past acute conditions that involved pig out crapulence, and 3) deaths caused by chronic conditions that involved medium (>1 to ≤2 drinks of alcohol [women] or >2 to ≤4 drinks [men]) Oregon high (>2 drinks of alcohol [women] or >4 drinks [men]) levels of average daily alcohol consumption.
Suggested citation for this article: Esser MB, Sherk A, Liu Y, et al. Deaths and Years of Potential Life story Lost From Excessive Alcohol Use — United States, 2011–2015. MMWR Morb Mortal Wkly Rep 2020;69:981–987. Department of the Interior: http://dx.DoI.org/10.15585/mmwr.mm6930a1external picture.
MMWR and Unwholesomeness and Mortality Weekly Cover are service marks of the U.S. Health and Human Services.
Use of trade names and commercial sources is for identification only and does non imply endorsement by the U.S. Department of Health and Hominine Services.
References to not-CDC sites happening the Internet are provided as a service to MMWR readers and serve not constitute operating theater imply warrant of these organizations or their programs away CDC or the U.S. Section of Wellness and Hominal Services. CDC is not creditworthy for the subject matter of pages found at these sites. URL addresses catalogued in MMWR were current atomic number 3 of the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This rebirth power result in character translation operating room format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR report copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.
alcohol related collisions cost the american public about 114
Source: https://www.cdc.gov/mmwr/volumes/69/wr/mm6930a1.htm
Posting Komentar untuk "alcohol related collisions cost the american public about 114"